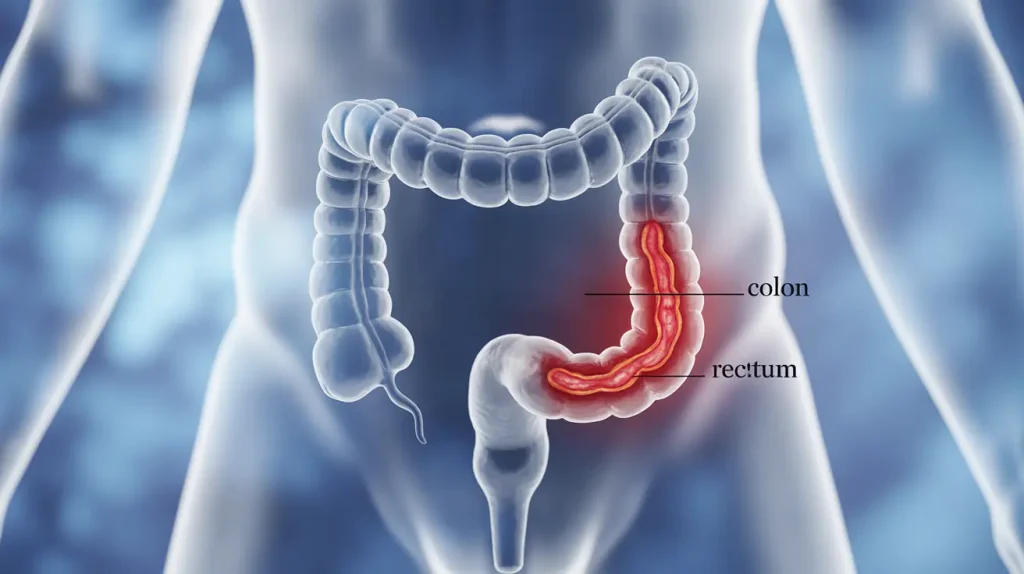
Ulcerative colitis is a chronic inflammatory bowel disease that causes long-lasting inflammation and ulcers in the digestive tract. This condition primarily affects the innermost lining of the large intestine, or the colon, and the rectum. Symptoms typically develop gradually rather than suddenly, and they vary depending on the severity of inflammation and its location. While the exact cause remains unknown, ulcerative colitis involves an abnormal immune system response. Here’s information about ulcerative colitis and how it is managed:
Diagnosing Ulcerative Colitis
Proper management of ulcerative colitis begins with an accurate and thorough diagnosis. There is currently no known cure, but various treatment approaches are available to help manage the symptoms and support daily physical function. Physicians can diagnose gastrointestinal conditions by:
- Assessing Medical History
- Taking Physical Examinations
- Ordering Specific Diagnostic Tests
Endoscopic procedures allow doctors to view the colon, and blood tests help identify potential markers of inflammation. A colonoscopy is a primary diagnostic tool for this health condition.
A colonoscopy procedure allows a physician to examine the entire colon using a thin, flexible, lighted tube equipped with a camera. During the procedure, the doctor can take small tissue samples for biopsy. These biopsies help rule out other similar conditions, such as Crohn’s disease, and confirm the specific presence of ulcerative colitis. Stool tests may also be utilized to check for underlying infections or concealed blood in the gastrointestinal tract.
Treating With Medication
After a diagnosis is made, healthcare providers often start with pharmacological therapies to reduce chronic inflammation and manage daily symptoms. The specific choice of medication depends on the severity of the condition and the individual patient’s physiological response. Aminosalicylates help reduce inflammation in the lining of the colon, and they are frequently prescribed for mild to moderate cases. These medications can be administered orally, via enema, or as a suppository, depending on the affected segment of the colon.
Corticosteroids may be added to a treatment plan when symptoms don’t respond to aminosalicylates, as corticosteroids also have anti-inflammatory properties. These powerful anti-inflammatory drugs are typically reserved for short-term use to control moderate to severe flare-ups. Prolonged use of corticosteroids is generally avoided due to their potential adverse side effects, so they are rarely used alone.
Immunosuppressants are another distinct pharmacological approach, which are used to suppress the immunological response causing inflammation. Instead of treating the inflammation directly, these medications target the underlying immune response contributing to symptoms. Patients taking immunosuppressant medications require regular medical monitoring, often including routine blood tests. Healthcare providers assess medications and treatment plans to verify they are working well without causing secondary complications.
Treating With Surgery
For certain individuals, medication may not provide adequate symptom control, or they cause too many side effects. In these specific situations, surgical intervention may be recommended. Surgery for ulcerative colitis generally involves removing the entire colon and rectum to eliminate the disease. A common surgical procedure is a proctocolectomy with an ileal pouch-anal anastomosis.
During this operation, the surgeon removes the colon and rectum entirely, constructing an internal pouch from the end of the small intestine. This pouch is then attached directly to the anus, allowing the patient to expel waste without the need for an external appliance. Another surgical option is a proctocolectomy combined with an ileostomy. The surgeon brings the end of the small intestine through an opening in the abdominal wall, and waste collects in an external bag. This secure medical appliance is worn outside the body and requires regular emptying and routine maintenance by the patient.
Learn More About Ulcerative Colitis
Navigating a chronic digestive illness requires ongoing education and close collaboration with specialized medical professionals. Treatment plans must be carefully individualized, as the condition affects every person differently. To learn more about your gastrointestinal health, ask your primary doctor about screening options at your next visit. You may need to contact your provider sooner to schedule a consultation if you are experiencing any abdominal symptoms. Consistent medical check-ups and open communication with a healthcare team will help you stay proactive about your overall health.