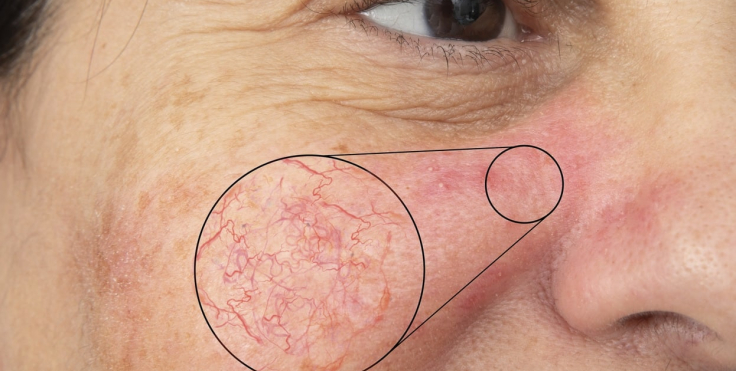
Spider veins are damaged veins that appear near the surface of the skin, usually appearing as thin, branching lines. They most often appear on the legs or face, where they can look similar to a spider web or tree branches. While they are usually only a cosmetic concern, understanding what causes them helps you make informed decisions about your care. Here’s information about spider veins and how you can manage them:
Spider Vein Causes
Veins carry blood back to the heart, working against gravity. Valves in your blood vessels keep blood flowing in the right direction, and damaged valves allow blood to pool near the surface of the skin. When this pooling occurs, the pressure causes the small vessels to expand and become visible. Several underlying factors contribute to this valve damage and the development of spider veins.
Genetics has a significant role, meaning you are more likely to develop them if your family members have them. Age also affects the veins, as normal wear and tear over time weakens the vessel walls and valves. Hormonal fluctuations, particularly during puberty, pregnancy, or menopause, can relax vein walls and increase susceptibility. Prolonged sitting or standing places extra pressure on the veins in your legs. If you work in an occupation that requires you to remain on your feet for long periods, you may be at an increased risk of vein issues.
Spider Vein Risks
While anyone can develop spider veins, certain groups face a higher risk. Advancing age remains one of the most prominent risk factors, as veins naturally lose their elasticity over time. Women experience this condition more frequently than men, largely due to the hormonal changes mentioned above.
Body weight also impacts vein health. Excess weight places additional pressure on the leg veins, making it harder for blood to flow upward. Pregnancy adds both extra weight and increased blood volume, which commonly leads to enlarged veins. A sedentary lifestyle further exacerbates the issue.
Certain lifestyle factors increase the likelihood of developing spider veins, but simple daily changes can help reduce these risks. Incorporating regular movement into your routine promotes better circulation and supports overall vein function. Addressing spider veins often begins with conservative management techniques. Reducing chronic venous insufficiency is a primary goal when managing vein health.
Spider Vein Treatment Options
Venous insufficiency is a medical condition in which the veins have difficulty returning blood from the lower extremities back to the heart. This issue arises when vein walls or valves become weakened or damaged, impairing their ability to effectively push blood upward against gravity. As a result, blood can pool in the veins, leading to swelling, pain, a heavy sensation in the legs, and sometimes visible varicose or spider veins. To manage spider veins, providers often recommend wearing compression stockings; these stockings apply gentle pressure, helping move blood more efficiently. Elevating your legs when resting and exercising regularly also supports proper blood flow.
If conservative measures do not alleviate your vein concerns, several more direct procedures are available. Sclerotherapy is a highly common procedure for this condition. During this treatment, a specialist injects a chemical solution directly into the affected vein. This solution irritates the lining of the blood vessel, causing it to collapse and eventually fade from view.
Doctors often recommend sclerotherapy for targeted treatment, or they may suggest laser therapy for smaller visible veins. The right approach depends on the size and location of the veins. After sclerotherapy, side effects may include redness, bruising, and pain in the treatment area, and brown spots are also common. You will be supervised by medical professionals for other less common effects, such as:
- Nausea
- Headaches
- Allergic Reaction
- Skin Discoloration
Manage Your Spider Veins Effectively
Addressing vein concerns requires accurate information and professional guidance. While many non-invasive methods can improve circulation, visible veins usually require specific interventions to fade completely. A trained medical professional can assess your specific situation and evaluate the health of your circulatory system. To learn about your options, contact a vein specialist for a consultation today. They will review your medical history, examine the affected areas, and discuss the most appropriate path forward.