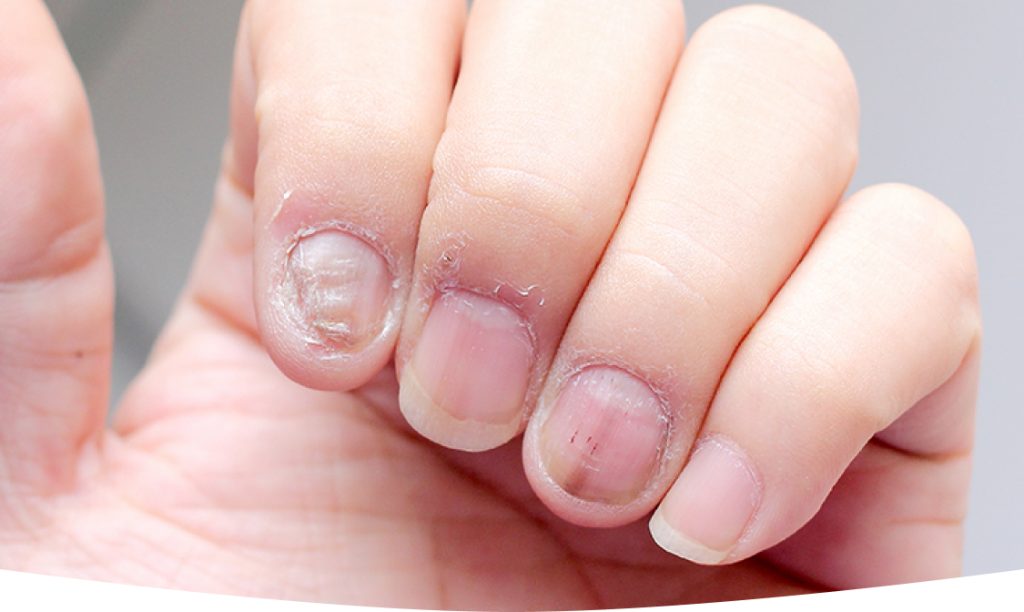
Fungal nails and infections involve the growth of fungi underneath or within the nail structure. These infections cause the nail to become discolored, thickened, and brittle over time. Early identification allows medical providers to address the infection promptly. Fungi break down the nail material, so the texture and appearance of the nail often change. Initial signs may include a small white or yellow spot on the nail, which can enlarge as the infection progresses. Identifying changes early helps guide treatment, and medical evaluation determines the appropriate approach.
What Are Fungal Nails?
A fungal nail is an infection affecting the hard nail structure. Fungi grow in dark, moist environments and survive by consuming keratin, which forms the nail’s main support. The infection weakens the nail, and the surface can turn yellow. Nails may thicken, and edges often become brittle or crumble. While the infection may start slowly, damage can accumulate over time, and in some cases, the nail separates from the underlying tissue. Debris sometimes forms under the nail, and the nail’s shape may change. Thickened nails can make trimming more difficult, and rough edges may catch on socks.
How Do Fungal Nails Develop?
Fungal nails with infections spread through contact with fungal organisms. The fungi thrive in warm, moist areas, and toenails provide an ideal environment for growth. Infection can develop when the fungi enter the nail through small cracks or damage. Shared nail instruments may transmit the fungus between individuals. Minor trauma to the nail can provide a site for fungal invasion. Fungal infections may start in the surrounding skin and move into the nail bed, causing nail changes. Moist, enclosed conditions support fungal growth, and repeated exposure to these environments increases the likelihood of infection.
How Are Fungal Nails Treated?
Treatment depends on the severity of the infection. Mild cases are often treated with topical antifungal medications applied directly to the nail. Because these treatments may not penetrate deeply, daily application over several months is usually necessary, and results can take time. More persistent infections may require oral antifungal medications. Oral therapy delivers medication through the bloodstream, and treatment duration is typically several months. Medical providers monitor patients regularly to assess effectiveness and adjust therapy if needed. Some cases may benefit from laser therapy, which targets fungal organisms using concentrated light. Severe infections may require partial or complete nail removal, allowing antifungal medication to reach the underlying tissue and supporting the growth of a healthy new nail.
Preventing fungal nails involves limiting exposure to environments where fungi thrive. Keeping feet clean and dry reduces fungal growth, and wearing breathable footwear allows moisture to escape. Regularly trimming nails straight across helps maintain healthy nail structure, and disinfecting nail tools reduces the risk of spreading fungal organisms. Avoiding prolonged exposure to damp areas, such as showers or locker rooms, lowers the likelihood of infection. These steps support nail health, and early attention to any nail changes can help prevent fungal infections from developing.
Find a Clinic
Early identification of fungal nail infections supports effective treatment. Medical evaluation helps determine the appropriate therapy, and prompt treatment improves outcomes. Topical, oral, and advanced medical options provide flexible approaches depending on infection severity. Consistent monitoring of nail changes ensures timely intervention, and following professional guidance helps manage the infection successfully. Maintaining nail health and addressing changes early reduces the risk of the infection advancing.